I’m a 15 year old girl and I regularly sleep 8 hours or more. However, I feel very tired during the day and I wake up feeling very groggy and unrested. My sister (who sleeps in the same room as ...
Thank you for your question! This article helps explain more about your symptoms: https://medicalchannelasia.com/moles-when-should-i-be-worried/ Moles in general are common skin growths that develop when melanocytes, pigment-producing cells in your skin, cluster together. These clusters cause the daRead more
Thank you for your question!
This article helps explain more about your symptoms:
https://medicalchannelasia.com/moles-when-should-i-be-worried/
Moles in general are common skin growths that develop when melanocytes, pigment-producing cells in your skin, cluster together. These clusters cause the darkening of the skin and can appear anywhere on your body, including the scalp, genitals, and inside your mouth.
Most moles are harmless and typically appear during childhood and adolescence. You can have anywhere from 10 to 40 moles by adulthood, and they may change in color, size, and texture over time. Some moles may even fade away completely.
Here are some characteristics of moles:
- Color: Moles can vary in color from light brown to black, pink, red, tan, or even blue.
- Size: Most moles are smaller than a pencil eraser (about 6 millimeters or ¼ inch in diameter).
- Shape: Moles can be round, oval, or irregular in shape.
- Texture: Moles can be flat, smooth, raised, or wrinkled. They may also have coarse hairs growing out of them.
While most moles are benign (noncancerous), some can be cancerous. Melanoma, the most serious type of skin cancer, can develop from a mole. Early detection is key to successful treatment, so it’s important to be aware of the signs and symptoms of melanoma.
Here are some tips for monitoring your moles:
- The ABCDE rule: This rule can help you identify moles that may be cancerous.
- Asymmetry: One half of the mole doesn’t match the other half.
- Border: The border of the mole is irregular, notched, or blurred.
- Color: The mole has more than one color, or the color changes within the mole.
- Diameter: The mole is larger than 6 millimeters (¼ inch) in diameter.
- Evolving: The mole is changing in size, shape, or color.
- Perform regular skin self-exams: Look for any new moles or changes in existing moles. Pay particular attention to moles in areas you don’t normally see, such as your back or scalp.
- See a doctor: If you notice any changes in a mole, see a doctor or dermatologist for a professional evaluation.
If you’re experiencing any skin issues, it is best to consult a Dermatologist doctor to determine the cause and receive proper treatment. This information from Medical Channel Asia is not a substitute for professional medical advice. Consulting a doctor is important to get a proper diagnosis and treatment plan.
See less
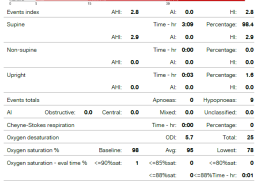
Feeling tired despite getting 8 hours of sleep and waking up groggy could indicate that your sleep quality, rather than the quantity, might be the issue. Snoring or loud breathing could be signs of a sleep-related problem, such as sleep apnea or other breathing disturbances. Here are some possibilitRead more
Feeling tired despite getting 8 hours of sleep and waking up groggy could indicate that your sleep quality, rather than the quantity, might be the issue. Snoring or loud breathing could be signs of a sleep-related problem, such as sleep apnea or other breathing disturbances. Here are some possibilities:
1. Sleep Apnea:
2. Sleep Hygiene:
3. Other Factors:
4. Medical Consultation:
If this fatigue is affecting your daily life or school performance, seeking advice sooner rather than later is a good idea.
https://www.helf.co/en
All responses provided by HELF are generated by its AI architecture. The information shared is intended for general informational purposes only and should not be relied upon for medical diagnosis or treatment. Please consult a healthcare provider for any medical concerns, diagnosis or treatment.
See less